Palonosetron Injection, Solution
FDA Label NDC 55111-694
Structured Product Label
The following Structured Product Label (SPL) was submitted to the FDA by Dr.reddy's Laboratories Limited for the product Palonosetron (NDC 55111-694). This document serves as the official prescribing information, containing essential scientific data and clinical materials required for healthcare providers and patients.
This specific version of the label includes detailed information regarding 1 indications and usage, 1.1 chemotherapy-induced nausea and vomiting in adults, 1.2 chemotherapy-induced nausea and vomiting in pediatric patients aged 1 month to less than 17 years, 1.3 postoperative nausea and vomiting in adults, 2 dosage and administration, 2.1 recommended dosing, 2.2 instructions for intravenous administration, 3 dosage forms and strengths, and other regulatory disclosures. Use the navigation below to review specific sections of the FDA submission.
Label Section Quick Index
1.1 Chemotherapy-Induced Nausea And Vomiting In Adults
Palonosetron hydrochloride injection is indicated for:
• Moderately emetogenic cancer chemotherapy -- prevention of acute and delayed nausea and vomiting associated with initial and repeat courses
• Highly emetogenic cancer chemotherapy -- prevention of acute nausea and vomiting associated with initial and repeat courses
1.2 Chemotherapy-Induced Nausea And Vomiting In Pediatric Patients Aged 1 Month To Less Than 17 Years
Pediatric use information is approved for Helsinn Healthcare SA’s palonosetron hydrochloride injection. However, due to Helsinn Healthcare SA’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
1.3 Postoperative Nausea And Vomiting In Adults
Palonosetron hydrochloride injection is indicated for prevention of postoperative nausea and vomiting (PONV) for up to 24 hours following surgery. Efficacy beyond 24 hours has not been demonstrated. As with other antiemetics, routine prophylaxis is not recommended in patients in whom there is little expectation that nausea and/or vomiting will occur postoperatively.
In patients where nausea and vomiting must be avoided during the postoperative period, palonosetron hydrochloride injection is recommended even where the incidence of postoperative nausea and/or vomiting is low.
2 Dosage And Administration
2.1 Recommended Dosing
Chemotherapy-Induced Nausea and Vomiting
| Age | Dose | Infusion Time |
| Adults | 0.25 mg x 1 | Infuse over 30 seconds beginning approx. 30 min before the start of chemo |
Pediatric use information for patents aged 1 month to less than 17 years is approved for Helsinn Healthcare SA’s palonosetron hydrochloride injection. However, due to Helsinn Healthcare SA’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
Postoperative Nausea and Vomiting
Dosage for Adults - a single 0.075 mg intravenous dose administered over 10 seconds immediately before the induction of anesthesia. .
2.2 Instructions For Intravenous Administration
Palonosetron hydrochloride injection is supplied ready for intravenous administration at a concentration of 0.05 mg/mL (50 mcg/ mL). Palonosetron hydrochloride injection should not bemixed with other drugs. The infusion line should be flushed with normal saline before and after administration of palonosetron hydrochloride injection. Parenteral drug products should be inspected visually for particulate matter and discoloration before administration, whenever solution and container permit.
3 Dosage Forms And Strengths
Palonosetron hydrochloride injection is supplied as a single-use sterile, clear, colorless solution in glass vials that provide:
• 0.25 mg (free base) per 5 mL (concentration: 0.05 mg/mL, 50 mcg/mL)
• 0.075 mg (free base) per 1.5 mL (concentration: 0.05 mg/mL, 50 mcg/mL)
4 Contraindications
Palonosetron hydrochloride injection is contraindicated in patients known to have hypersensitivity to the drug or any of its components. [see Adverse Reactions (6.2)]
5 Warnings And Precautions
5.1 Hypersensitivity
Hypersensitivity reactions, including anaphylaxis, have been reported with or without known hypersensitivity to other 5-HT3 receptor antagonists.
5.2 Serotonin Syndrome
The development of serotonin syndrome has been reported with 5-HT3 receptor antagonists. Most reports have been associated with concomitant use of serotonergic drugs (e.g., selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), monoamine oxidase inhibitors, mirtazapine, fentanyl, lithium, tramadol, and intravenous methylene blue). Some of the reported cases were fatal. Serotonin syndrome occurring with overdose of another 5-HT3 receptor antagonist alone has also been reported. The majority of reports of serotonin syndrome related to 5-HT3 receptor antagonist use occurred in a post-anesthesia care unit or an infusion center.
Symptoms associated with serotonin syndrome may include the following combination of signs and symptoms: mental status changes (e.g. agitation, hallucinations, delirium, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular symptoms (e.g., tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, with or without gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea). Patients should be monitored for the emergence of serotonin syndrome, especially with concomitant use of palonosetron hydrochloride injection and other serotonergic drugs. If symptoms of serotonin syndrome occur, discontinue palonosetron hydrochloride injection and initiate supportive treatment. Patients should be informed of the increased risk of serotonin syndrome, especially if palonosetron hydrochloride injection is used concomitantly with other serotonergic drugs [see Drug Interactions (7), Patient Counseling Information (17)].
6 Adverse Reactions
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
6.1 Chemotherapy-Induced Nausea And Vomiting
Adults
In clinical trials for the prevention of nausea and vomiting induced by moderately or highly emetogenic chemotherapy, 1374 adult patients received palonosetron. Adverse reactions were similar in frequency and severity with palonosetron hydrochloride injection and ondansetron or dolasetron. Following is a listing of all adverse reactions reported by ≥ 2% of patients in these trials (Table 1).
Table 1: Adverse Reactions from Chemotherapy-Induced Nausea and Vomiting Studies ≥ 2% in any Treatment Group
| Event | Palonosetron hydrochloride injection 0.25 mg(N=633) | Ondansetron 32 mg I.V. (N=410) | Dolasetron 100 mg I.V.(N=194) |
| Headache | 60 (9%) | 34 (8%) | 32 (16%) |
| Constipation | 29 (5%) | 8 (2%) | 12 (6%) |
| Diarrhea | 8 (1%) | 7 (2%) | 4 (2%) |
| Dizziness | 8 (1%) | 9 (2%) | 4 (2%) |
| Fatigue | 3 (< 1%) | 4 (1%) | 4 (2%) |
| Abdominal Pain | 1 (< 1%) | 2 (< 1%) | 3 (2%) |
| Insomnia | 1 (< 1%) | 3 (1%) | 3 (2%) |
In other studies, 2 subjects experienced severe constipation following a single palonosetron dose of approximately 0.75 mg, three times the recommended dose. One patient received a 10 mcg/kg oral dose in a post operative nausea and vomiting study and one healthy subject received a 0.75 mg I.V. dose in a pharmacokinetic study.
In clinical trials, the following infrequently reported adverse reactions, assessed by investigators as treatment-related or causality unknown, occurred following administration of palonosetron hydrochloride injection to adult patients receiving concomitant cancer chemotherapy:
Cardiovascular: 1%: non-sustained tachycardia, bradycardia, hypotension, < 1%: hypertension, myocardial ischemia, extrasystoles, sinus tachycardia, sinus arrhythmia, supraventricular extrasystoles and QT prolongation. In many cases, the relationship to palonosetron hydrochloride injection was unclear.
Dermatological: < 1%: allergic dermatitis, rash.
Hearing and Vision: < 1%: motion sickness, tinnitus, eye irritation and amblyopia.
Gastrointestinal System: 1%: diarrhea, < 1%: dyspepsia, abdominal pain, dry mouth, hiccups and flatulence.
General: 1%: weakness, < 1%: fatigue, fever, hot flash, flu-like syndrome.
Liver: < 1%: transient, asymptomatic increases in AST and/or ALT and bilirubin. These changes occurred predominantly in patients receiving highly emetogenic chemotherapy.
Metabolic: 1%: hyperkalemia, < 1%: electrolyte fluctuations, hyperglycemia, metabolic acidosis, glycosuria, appetite decrease, anorexia.
Musculoskeletal: < 1%: arthralgia.
Nervous System: 1%: dizziness, < 1%: somnolence, insomnia, hypersomnia, paresthesia.
Psychiatric: 1%: anxiety, < 1%: euphoric mood.
Urinary System: < 1%: urinary retention.
Vascular: < 1%: vein discoloration, vein distention.
Pediatrics
The following adverse reactions were reported for palonosetron:
Nervous System: <1%: headache, dizziness, dyskinesia.
General: <1%: infusion site pain.
Dermatological: <1%: allergic dermatitis, skin disorder.
Pediatric use information for patents aged 1 month to less than 17 years is approved for Helsinn Healthcare SA’s palonosetron hydrochloride injection. However, due to Helsinn Healthcare SA’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
6.2 Postoperative Nausea And Vomiting
The adverse reactions cited in Table 2 were reported in ≥ 2% of adults receiving I.V. Palonosetron hydrochloride injection 0.075 mg immediately before induction of anesthesia in one phase 2 and two phase 3 randomized placebo-controlled trials. Rates of events between palonosetron and placebo groups were similar. Some events are known to be associated with, or may be exacerbated by concomitant perioperative and intraoperative medications administered in this surgical population. Please refer to Section 12.2, thorough QT/QTc study results, for data demonstrating the lack of palonosetron effect on QT/QTc.
Table 2: Adverse Reactions from Postoperative Nausea and Vomiting Studies ≥ 2% in any Treatment Group
| Event | Palonosetron hydrochloride injection 0.075 mg (N=336) | Placebo (N=369) |
| ElectrocardiogramQT prolongation | 16 (5%) | 11 (3%) |
| Bradycardia | 13 (4%) | 16 (4%) |
| Headache | 11 (3%) | 14 (4%) |
| Constipation | 8 (2%) | 11(3%) |
In these clinical trials, the following infrequently reported adverse reactions, assessed by investigators as treatment-related or causality unknown, occurred following administration of palonosetron hydrochloride injection to adult patients receiving concomitant perioperative and intraoperative medications including those associated with anesthesia:
Cardiovascular: 1%: electrocardiogram QTc prolongation, sinus bradycardia, tachycardia, < 1%: blood pressure decreased, hypotension, hypertension, arrhythmia, ventricular extrasystoles, generalized edema, ECG T wave amplitude decreased, platelet count decreased. The frequency of these adverse effects did not appear to be different from placebo.
Dermatological: 1%: pruritus.
Gastrointestinal System: 1%: flatulence, < 1%: dry mouth, upper abdominal pain, salivary hypersecretion, dyspepsia, diarrhea, intestinal hypomotility, anorexia.
General: < 1%: chills.
Liver: 1%: increases in AST and/or ALT, < 1%: hepatic enzyme increased.
Metabolic: < 1%: hypokalemia, anorexia.
Nervous System: < 1%: dizziness.
Respiratory: < 1%: hypoventilation, laryngospasm.
Urinary System: 1%: urinary retention.
6.3 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of palonosetron hydrochloride injection. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Very rare cases (<1/10,000) of hypersensitivity reactions including anaphylaxis and anaphylactic shock and injection site reactions (burning, induration, discomfort and pain) were reported from postmarketing experience of palonosetron hydrochloride injection 0.25 mg in the prevention of chemotherapy-induced nausea and vomiting.
7 Drug Interactions
Palonosetron is eliminated from the body through both renal excretion and metabolic pathways with the latter mediated via multiple CYP enzymes. Further in vitro studies indicated that palonosetron is not an inhibitor of CYP1A2, CYP2A6, CYP2B6, CYP2C9, CYP2D6, CYP2E1 and CYP3A4/5 (CYP2C19 was not investigated) nor does it induce the activity of CYP1A2, CYP2D6, or CYP3A4/5. Therefore, the potential for clinically significant drug interactions with palonosetron appears to be low.
Serotonin syndrome (including altered mental status, autonomic instability, and neuromuscular symptoms) has been described following the concomitant use of 5-HT3 receptor antagonists and other serotonergic drugs, including selective serotonin reuptake inhibitors (SSRIs) and serotonin and noradrenaline reuptake inhibitors (SNRIs) [see Warnings and Precautions (5.2)].
Coadministration of 0.25 mg I.V. palonosetron and 20 mg I.V. dexamethasone in healthy subjects revealed no pharmacokinetic drug- interactions between palonosetron and dexamethasone.
In an interaction study in healthy subjects where palonosetron 0.25 mg (I.V. bolus) was administered on day 1 and oral aprepitant for 3 days (125 mg/80 mg/80 mg), the pharmacokinetics of palonosetron were not significantly altered (AUC: no change, Cmax: 15% increase).
A study in healthy volunteers involving single-dose I.V. palonosetron (0.75 mg) and steady state oral metoclopramide (10 mg four times daily) demonstrated no significant pharmacokinetic interaction.
In controlled clinical trials, palonosetron hydrochloride injection has been safely administered with corticosteroids, analgesics, antiemetics/antinauseants, antispasmodics and anticholinergic agents.
Palonosetron did not inhibit the antitumor activity of the five chemotherapeutic agents tested (cisplatin, cyclophosphamide, cytarabine, doxorubicin and mitomycin C) in murine tumor models.
8 Use In Specific Populations
8.1 Pregnancy
Pregnancy Category B
Risk Summary
Adequate and well controlled studies with palonosetron hydrochloride injection have not beenconducted in pregnant women. In animal reproduction studies, no effects on embryo-fetal development were observed with the administration of oral palonosetron during the period of organogenesis at doses up to 1894 and 3789 times the recommended human intravenous dose in rats and rabbits, respectively. Because animal reproduction studies are not always predictive of human response, palonosetron hydrochloride injection should be used during pregnancy only if clearly needed.
Animal Data
In animal studies, no effects on embryo-fetal development were observed in pregnant rats given oral palonosetron at doses up to 60 mg/kg/day (1894 times the recommended human intravenous dose based on body surface area) or pregnant rabbits given oral doses up to 60 mg/kg/day (3789 times the recommended human intravenous dose based on body surface area) during the period of organogenesis.
8.3 Nursing Mothers
It is not known whether palonosetron hydrochloride injection is present in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants and the potential for tumorigenicity shown for palonosetron in the rat carcinogenicity study [see Nonclinical Toxicology (13.1)], a decision should be made whether todiscontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
8.4 Pediatric Use
Chemotherapy-Induced Nausea and Vomiting
Safety and effectiveness of palonosetron hydrochloride injection in neonates (less than 1 month of age) have not been established.
Pediatric use information for patents aged 1 month to less than 17 years is approved for Helsinn Healthcare SA’s palonosetron hydrochloride injection. However, due to Helsinn Healthcare SA’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
Postoperative Nausea and Vomiting Studies
Safety and efficacy have not been established in pediatric patients for prevention of postoperative nausea and vomiting.
Additional information regarding a clinical study in which efficacy was not demonstrated in patients aged 1 month to less than 17 years is included in the package insert for Helsinn Healthcare SA’s palonosetron hydrochloride injection. However, due toHelsinn Healthcare SA’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
8.5 Geriatric Use
Population pharmacokinetics analysis did not reveal any differences in palonosetron pharmacokinetics between cancer patients ≥ 65 years of age and younger patients (18 to 64 years). Of the 1374 adult cancer patients in clinical studies of palonosetron, 316 (23%) were ≥ 65 years old, while 71 (5%) were ≥ 75 years old. No overall differences in safety or effectiveness were observed between these subjects and the younger subjects, but greater sensitivity in some older individuals cannot be ruled out. No dose adjustment or special monitoring are required for geriatric patients.
Of the 1520 adult patients in palonosetron hydrochloride injection PONV clinical studies, 73 (5%) were ≥65 years old. No overall differences in safety were observed between older and younger subjects in these studies, though the possibility of heightened sensitivity in some older individuals cannot be excluded. No differences in efficacy were observed in geriatric patients for the CINV indication and none are expected for geriatric PONV patients. However, Palonosetron hydrochloride injection efficacy in geriatric patients has not been adequately evaluated.
8.6 Renal Impairment
Mild to moderate renal impairment does not significantly affect palonosetron pharmacokinetic parameters. Total systemic exposure increased by approximately 28% in severe renal impairment relative to healthy subjects. Dosage adjustment is not necessary in patients with any degree of renal impairment.
8.7 Hepatic Impairment
Hepatic impairment does not significantly affect total body clearance of palonosetron compared to the healthy subjects. Dosage adjustment is not necessary in patients with any degree of hepatic impairment.
8.8 Race
Intravenous palonosetron pharmacokinetics was characterized in twenty-four healthy Japanese subjects over the dose range of 3–90 mcg/kg. Total body clearance was 25% higher in Japanese subjects compared to Whites, however, no dose adjustment is required. The pharmacokinetics of palonosetron in Blacks has not been adequately characterized.
10 Overdosage
There is no known antidote to palonosetron hydrochloride injection. Overdose should be managed with supportive care.
Fifty adult cancer patients were administered palonosetron at a dose of 90 mcg/kg (equivalent to 6 mg fixed dose) as part of a dose ranging study. This is approximately 25 times the recommended dose of 0.25 mg. This dose group had a similar incidence of adverse events compared to the other dose groups and no dose response effects were observed.
Dialysis studies have not been performed, however, due to the large volume of distribution, dialysis is unlikely to be an effective treatment for palonosetron overdose. A single intravenous dose of palonosetron at 30 mg/kg (947 and 474 times the human dose for rats and mice, respectively, based on body surface area) was lethal to rats and mice. The major signs of toxicity were convulsions, gasping, pallor, cyanosis and collapse.
11 Description
Palonosetron hydrochloride is an antiemetic and antinauseant agent. It is a serotonin-3 (5-HT3) receptor antagonist with a strong binding affinity for this receptor. Chemically, palonosetron hydrochloride is: (3aS)-2-[(S)-1-Azabicyclo [2.2.2]oct-3-yl]-2,3,3a,4,5,6-hexahydro-1-oxo- 1Hbenz[de]isoquinoline hydrochloride. The empirical formula is C19H24N2O.HCl, with a molecular weight of 332.87. Palonosetron hydrochloride exists as a single isomer and has the following structural formula:
Palonosetron hydrochloride is a white to off-white crystalline powder. It is freely soluble in water and soluble in methanol.
Palonosetron hydrochloride injection is a sterile, clear, colorless, non pyrogenic, isotonic, buffered solution for intravenous administration. Palonosetron hydrochloride injection is available as 5 mL single use vial or 1.5 mL single use vial.
Each 5 mL vial contains 0.25 mg palonosetron base as hydrochloride, 207.5 mg mannitol, disodium edetate and sodium acetate trihydrate in water for intravenous administration.
Each 1.5 mL vial contains 0.075 mg palonosetron base as hydrochloride, 62.25 mg mannitol, disodium edetate and sodium acetate trihydrate in water for intravenous administration.
The pH of the solution in the 5 mL and 1.5 mL vials is 4.5 to 5.5, Hydrochloric acid or sodium hydroxide may have been added to adjust pH.
12 Clinical Pharmacology
12.1 Mechanism Of Action
Palonosetron is a 5-HT3 receptor antagonist with a strong binding affinity for this receptor and little or no affinity for other receptors.
Cancer chemotherapy may be associated with a high incidence of nausea and vomiting, particularly when certain agents, such as cisplatin, are used. 5-HT3 receptors are located on the nerve terminals of the vagus in the periphery and centrally in the chemoreceptor trigger zone of the area postrema. It is thought that chemotherapeutic agents produce nausea and vomiting by releasing serotonin from the enterochromaffin cells of the small intestine and that the released serotonin then activates 5-HT3 receptors located on vagal afferents to initiate the vomiting reflex.
Postoperative nausea and vomiting is influenced by multiple patient, surgical and anesthesia related factors and is triggered by release of 5-HT in a cascade of neuronal events involving both the central nervous system and the gastrointestinal tract. The 5-HT3 receptor has been demonstrated to selectively participate in the emetic response.
12.2 Pharmacodynamics
The effect of palonosetron on blood pressure, heart rate, and ECGparameters including QTc were comparable to ondansetron and dolasetron in CINV clinical trials. In PONV clinical trials the effect of palonosetron on the QTc interval was no different from placebo. In non-clinical studies palonosetron possesses the ability to block ion channels involved in ventricular de- and re-polarization and to prolong action potential duration.
The effect of palonosetron on QTc interval was evaluated in a double blind, randomized, parallel, placebo and positive (moxifloxacin) controlled trial in adult men and women. The objective was to evaluate the ECG effects of I.V. administered palonosetron at single doses of 0.25, 0.75 or 2.25 mg in 221 healthy subjects. The study demonstrated no significant effect on any ECG interval including QTc duration (cardiac repolarization) at doses up to 2.25 mg.
12.3 Pharmacokinetics
After intravenous dosing of palonosetron in healthy subjects and cancer patients, an initial decline in plasma concentrations is followed by a slow elimination from the body. Mean maximum plasma concentration (Cmax) and area under the concentration-time curve (AUC0-∞) are generally dose- proportional over the dose range of 0.3–90 mcg/kg in healthy subjects and in cancer patients. Following single I.V. dose of palonosetron at 3 mcg/kg (or 0.21 mg/70 kg) to six cancer patients, mean (±SD) maximum plasma concentration was estimated to be 5630 ± 5480 ng/L and mean AUC was 35.8 ± 20.9 h•mcg/L.
Following I.V. administration of palonosetron 0.25 mg once every other day for 3 doses in 11 cancer patients, the mean increase in plasma palonosetron concentration from Day 1 to Day 5 was 42±34%. Following I.V. administration of palonosetron 0.25 mg once daily for 3 days in 12 healthy subjects, the mean (±SD) increase in plasma palonosetron concentration from Day 1 to Day 3 was 110±45%.
After intravenous dosing of palonosetron in patients undergoing surgery (abdominal surgery or vaginal hysterectomy), the pharmacokinetic characteristics of palonosetron were similar to those observed in cancer patients.
Distribution
Palonosetron has a volume of distribution of approximately 8.3 ±2.5 L/kg. Approximately 62% of palonosetron is bound to plasma proteins.
Metabolism
Palonosetron is eliminated by multiple routes with approximately 50% metabolized to form two primary metabolites: N-oxide-palonosetron and 6-S hydroxy-palonosetron. These metabolites each have less than 1% of the 5 HT3 receptor antagonist activity of palonosetron. In vitro metabolism studies have suggested that CYP2D6 and to a lesser extent, CYP3A4 and CYP1A2 are involved in the metabolism of palonosetron. However, clinical pharmacokinetic parameters are not significantly different between poor and extensive metabolizers of CYP2D6 substrates.
Elimination
After a single intravenous dose of 10 mcg/kg [14C]-palonosetron, approximately 80% of the dose was recovered within 144 hours in the urine with palonosetron representing approximately 40% of the administered dose. In healthy subjects, the total body clearance of palonosetron was 0.160 ± 0.035 L/h/kg and renal clearance was 0.067± 0.018 L/h/kg. Mean terminal elimination half-life is approximately 40 hours
Special Populations
Pediatric Patients
Pediatric use information for patents aged 1 month to less than 17 years is approved for Helsinn Healthcare SA’s palonosetron hydrochloride injection. However, due to Helsinn Healthcare SA’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
13 Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment Of Fertility
In a 104-week carcinogenicity study in CD-1 mice, animals were treated with oral doses of palonosetron at 10, 30 and 60 mg/kg/day. Treatment with palonosetron was not tumorigenic. The highest tested dose produce a systemic exposure to palonosetron (Plasma AUC) of about 150 to 289 times the human exposure (AUC= 29.8 h•mcg/L) at the recommended intravenous dose of 0.25 mg. In a 104-week carcinogenicity study in Sprague-Dawley rats, male and female rats were treated with oral doses of 15, 30 and 60 mg/kg/day and 15, 45 and 90 mg/kg/day, respectively. The highest doses produced a systemic exposure to palonosetron (Plasma AUC) of 137 and 308 times the human exposure at the recommended dose. Treatment with palonosetron produced increased incidences of adrenal benign pheochromocytoma and combined benign and malignant pheochromocytoma, increased incidences of pancreatic Islet cell adenoma and combined adenoma and carcinoma and pituitary adenoma in male rats. In female rats, it produced hepatocellular adenoma and carcinoma and increased the incidences of thyroid C-cell adenoma and combined adenoma and carcinoma.
Palonosetron was not genotoxic in the Ames test, the Chinese hamster ovarian cell (CHO/HGPRT) forward mutation test, the ex vivo hepatocyte unscheduled DNA synthesis (UDS) test or the mouse micronucleus test. It was, however, positive for clastogenic effects in the Chinese hamster ovarian (CHO) cell chromosomal aberration test.
Palonosetron at oral doses up to 60 mg/kg/day (about 1894 times the recommended human intravenous dose based on body surface area) was found to have no effect on fertility and reproductive performance of male and female rats.
14 Clinical Studies
14.1 Chemotherapy Induced Nausea And Vomiting In Adultss
Efficacy of single-dose palonosetron injection in preventing acute and delayed nausea and vomiting induced by both moderately and highly emetogenic chemotherapy was studied in three Phase 3 trials and one Phase 2 trial. In these double-blind studies, complete response rates (no emetic episodes and no rescue medication) and other efficacy parameters were assessed through at least 120 hours after administration of chemotherapy. The safety and efficacy of palonosetron in repeated courses of chemotherapy was also assessed.
Moderately Emetogenic Chemotherapy
Two Phase 3, double-blind trials involving 1132 patients compared single-dose I.V. Palonosetron hydrochloride injection with either single-dose I.V. ondansetron (study 1) or dolasetron (study 2) given 30 minutes prior to moderately emetogenic chemotherapy including carboplatin, cisplatin ≤ 50 mg/m², cyclophosphamide < 1500 mg/m², doxorubicin > 25 mg/m², epirubicin, irinotecan, and methotrexate > 250 mg/m². Concomitant corticosteroids were not administered prophylactically in study 1 and were only used by 4-6% of patients in study 2. The majority of patients in these studies were women (77%), White (65%) and naïve to previous chemotherapy (54%). The mean age was 55 years.
Highly Emetogenic Chemotherapy
A Phase 2, double-blind, dose-ranging study evaluated the efficacy of single-dose I.V. palonosetron from 0.3 to 90 mcg/kg (equivalent to < 0.1 mg to 6 mg fixed dose) in 161 chemotherapy-naïve adult cancer patients receiving highly-emetogenic chemotherapy (either cisplatin ≥ 70 mg/m² or cyclophosphamide > 1100 mg/m²). Concomitant corticosteroids were not administered prophylactically. Analysis of data from this trial indicates that 0.25 mg is the lowest effective dose in preventing acute nausea and vomiting induced by highly emetogenic chemotherapy.
A Phase 3, double-blind trial involving 667 patients compared single- dose I.V. palonosetron hydrochloride injection with single-dose I.V. ondansetron (study 3) given 30 minutes prior to highly emetogenic chemotherapy including cisplatin ≥ 60 mg/m², cyclophosphamide > 1500 mg/m², and dacarbazine. Corticosteroids were co-administered prophylactically before chemotherapy in 67% of patients. Of the 667 patients, 51% were women, 60% White, and 59% naïve to previous chemotherapy. The mean age was 52 years.
Efficacy Results
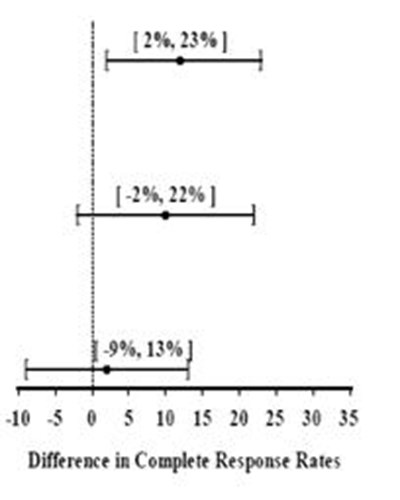
The antiemetic activity of palonosetron hydrochloride injection was evaluated during the acute phase (0-24 hours) [Table 4], delayed phase (24-120 hours) [Table 5], and overall phase (0-120 hours) [Table 6] post-chemotherapy in Phase 3 trials.
Table 4: Prevention of Acute Nausea and Vomiting (0-24 hours): Complete Response Rates
| Chemotherapy | Study | TreatmentGroup | Na | % with Complete Response | p-valueb | 97.5% Confidence Interval Palonosetron Hydrochloride Injection minus Comparatorc |
|---|---|---|---|---|---|---|
| ModeratelyEmetogenic | 1 | Palonosetron Hydrochloride 0.25 mg | 189 | 81 | 0.009 | |
| Ondansetron 32 mg I.V. | 185 | 69 | ||||
| 2 | Palonosetron Hydrochloride0.25 mg | 189 | 63 | NS | ||
| Dolasetron 100 mg I.V. | 191 | 53 | ||||
| Highly Emetogenic | 3 | Palonosetron Hydrochloride 0.25 mg | 223 | 59 | NS | |
| Ondansetron 32 mg I.V. | 221 | 57 |
a Intent-to-treat cohort
b 2-sided Fisher’s exact test. Significance level at α=0.025.
c These studies were designed to show non-inferiority. A lower bound greater than –15% demonstrates non- inferiority between palonosetron hydrochloride injection and comparator.
These studies show that palonosetron hydrochloride injection was effective in the prevention of acute nausea and vomiting associated with initial and repeat courses of moderately and highly emetogenic cancer chemotherapy. In study 3, efficacy was greater when prophylactic corticosteroids were administered concomitantly. Clinical superiority over other 5-HT3 receptor antagonists has not been adequately demonstrated in the acute phase.
Table 5: Prevention of Delayed Nausea and Vomiting (24-120 hours): Complete Response Rates
| Chemotherapy | Study | Treatment Group | Na | % with Complete Response | p-valueb | 97.5% Confidence Interval ALOXI minus Comparatorc |
|---|---|---|---|---|---|---|
| ModeratelyEmetogenic | 1 | Palonosetron Hydrochloride 0.25 mg | 189 | 74 | <0.001 | |
| Ondansetron 32 mg I.V. | 185 | 55 | ||||
| 2 | Palonosetron Hydrochloride 0.25 mg | 189 | 54 | 0.004 | ||
| Dolasetron 100 mg I.V. | 191 | 39 |
a Intent-to-treat cohort
b 2-sided Fisher’s exact test. Significance level at α=0.025.
c These studies were designed to show non-inferiority. A lower bound greater than –15% demonstrates non-inferiority between palonosetron hydrochloride injection and comparator.
These studies show that palonosetron hydrochloride injection was effective in the prevention of delayed nausea and vomiting associated with initial and repeat courses of moderately emetogenic chemotherapy.
Table 6: Prevention of Overall Nausea and Vomiting (0-120 hours): Complete Response Rates
| Chemotherapy | Study | TreatmentGroup | Na | % with Complete Response | p-valueb | 97.5% Confidence Interval Palonosetron Hydrochloride Injection minus Comparatorc |
|---|---|---|---|---|---|---|
| ModeratelyEmetogenic | 1 | Palonosetron Hydrochloride 0.25 mg | 189 | 69 | <0.001 | |
| Ondansetron 32 mg I.V. | 185 | 50 | ||||
| 2 | Palonosetron Hydrochloride 0.25 mg | 189 | 46 | 0.021 | ||
| Dolasetron 100 mg I.V. | 191 | 34 |
a Intent-to-treat cohort
b 2-sided Fisher’s exact test. Significance level at α=0.025.
c These studies were designed to show non-inferiority. A lower bound greater than –15% demonstrates non- inferiority between palonosetron hydrochloride injection and comparator.
These studies show that palonosetron hydrochloride injection was effective in the prevention of nausea and vomiting throughout the 120 hours (5 days) following initial and repeat courses of moderately emetogenic cancer chemotherapy.
14.2 Chemotherapy-Induced Nausea And Vomiting In Pediatrics
Pediatric use information for patents aged 1 month to less than 17 years is approved for Helsinn Healthcare SA’s palonosetron hydrochloride injection. However, due to Helsinn Healthcare SA’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
14.3 Postoperative Nausea And Vomiting
In one multicenter, randomized, stratified, double-blind, parallel-group, phase 3 clinical study (Study 1), palonosetron was compared with placebo for the prevention of PONV in 546 patients undergoing abdominal and gynecological surgery. All patients received general anesthesia. Study 1 was a pivotal study conducted predominantly in the US in the out-patient setting for patients undergoing elective gynecologic or abdominal laparoscopic surgery and stratified at randomization for the following risk factors: gender, non-smoking status, history of post operative nausea and vomiting and/or motion sickness.
In Study 1 patients were randomized to receive palonosetron 0.025 mg, 0.050 mg or 0.075 mg or placebo, each given intravenously immediately prior to induction of anesthesia. The antiemetic activity of palonosetron was evaluated during the 0 to 72 hour time period after surgery.
Of the 138 patients treated with 0.075 mg palonosetron in Study 1 and evaluated for efficacy, 96% were women; 66% had a history of PONV or motion sickness; 85% were non-smokers. As for race, 63% were White, 20% were Black, 15% were Hispanic, and 1% were Asian. The age of patients ranged from 21 to 74 years, with a mean age of 37.9 years. Three patients were greater than 65 years of age.
Co-primary efficacy measures were Complete Response (CR) defined as no emetic episode and no use of rescue medication in the 0-24 and in the 24-72 hours postoperatively.
Secondary efficacy endpoints included:
• Complete Response (CR) 0-48 and 0-72 hours
• Complete Control (CC) defined as CR and no more than mild nausea
• Severity of nausea (none, mild, moderate, severe)
The primary hypothesis in Study 1 was that at least one of the three palonosetron doses were superior to placebo.
Results for Complete Response in Study 1 for 0.075 mg palonosetron versus placebo are described in the following table.
Table 8: Prevention of Postoperative Nausea and Vomiting: Complete Response (CR), Study 1, Palonosetron 0.075 mg Vs Placebo
| Treatment | n/N (%) | Palonosetron Vs Placebo | |
|---|---|---|---|
| Δ | p-value* | ||
| Co-primary Endpoints | |||
| CR 0-24 hours | |||
| Palonosetron | 59/138 (42.8%) | 16.8% | 0.004 |
| Placebo | 35/135 (25.9%) | ||
| CR 24-72 hours | |||
| Palonosetron | 67/138 (48.6%) | 7.8% | 0.188 |
| Placebo | 55/135 (40.7%) | ||
* To reach statistical significance for each co-primary endpoint, the required significance limit for the lowest p-value was p<0.017.
Δ Difference (%): palonosetron 0.075 mg minus placebo
Palonosetron 0.075 mg reduced the severity of nausea compared to placebo. Analyses of other secondary endpoints indicate that palonosetron 0.075 mg was numerically better than placebo, however, statistical significance was not formally demonstrated.
A phase 2 randomized, double-blind, multicenter, placebo-controlled, dose ranging study was performed to evaluate I.V. palonosetron for the prevention of post-operative nausea and vomiting following abdominal or vaginal hysterectomy. Five I.V. palonosetron doses (0.1, 0.3, 1.0, 3.0 and 30 µg/kg) were evaluated in a total of 381 intent-to-treat patients. The primary efficacy measure was the proportion of patients with CR in the first 24 hours after recovery from surgery. The lowest effective dose was palonosetron 1µg/kg (approximately 0.075 mg) which had a CR rate of 44% versus 19% for placebo, p=0.004. Palonosetron 1 µg/kg also significantly reduced the severity of nausea versus placebo, p=0.009.
16 How Supplied/Storage And Handling
Palonosetron Hydrochloride Injection 0.075 mg/1.5 mL (free base) single-use vial packaged in a carton containing 5 vials. NDC 55111-694-19
Palonosetron Hydrochloride Injection 0.25 mg/5 mL (free base) single-use vial packaged in a carton containing 1 vial. NDC 55111-694-07
Storage
• Store at 20° to 25°C (68° to 77°F); [See USP Controlled Room Temperature].
• Protect from freez ing.
• Protect from light.
17 Patient Counseling Information
See FDA-approved patient labelling (Patient Information).
Instructions for Patients
Patients should be advised to report to their physician all of their medical conditions, including any pain, redness, or swelling in and around the infusion site [see Adverse Reactions (6.3)].
Advise patients of the possibility of serotonin syndrome, especially with concomitant use of palonosetron hydrochloride injection and another serotonergic agent such as medications to treat depression and migraines. Advise patients to seek immediate medical attention if the following symptoms occur: changes in mental status, autonomic instability, neuromuscular symptoms with or without gastrointestinal symptoms [see Warnings and Precautions (5.2)].
Patients should be instructed to read the Patient Information.
Package Label.Principal Display Panel Section
* Please review the disclaimer below.